Deerfield-News.com-Deerfield Beach, Fl-There currently are Four health-related issues occurring. The ground beef and cut fruits have not presented themselves yet in Florida according to the CDC.
Measles and Hepatitis A have both presented in Broward County.
Measles while currently, the State of Florida Department of Health lists as only one. Sources say that case is in Broward County. In 2018 we had a spike to a high of 15 cases in Broward.
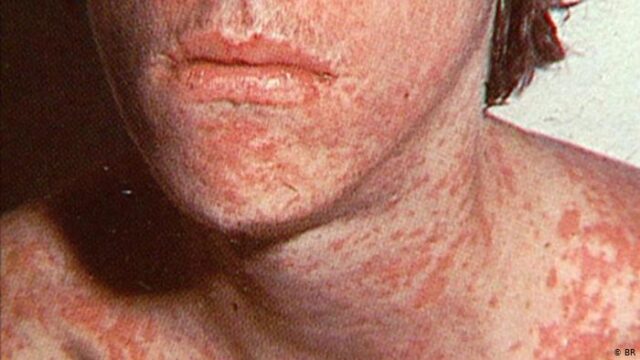
Measles
March Key Points
case
identified
documented vaccination
 In March 2019, 1 measles case was reported. Fewer than 10 cases were reported each year from 2013 to 2017, and a total of 15 cases were reported in 2018.
In March 2019, 1 measles case was reported. Fewer than 10 cases were reported each year from 2013 to 2017, and a total of 15 cases were reported in 2018.
So far in 2019, one Florida resident has spent time in Florida while infectious.
 A total of 138 people who had possible exposure to the measles case have been identified during this ongoing investigation. There were 2 main exposure settings, with the most contacts identified in health care settings.
A total of 138 people who had possible exposure to the measles case have been identified during this ongoing investigation. There were 2 main exposure settings, with the most contacts identified in health care settings.
Contact investigations are conducted to determine the vaccination status of those potentially exposed to measles, identify new cases, and prevent further transmission.
 Vaccination is the best way to prevent measles infections. In March, the case was not known to be vaccinated against measles.
Vaccination is the best way to prevent measles infections. In March, the case was not known to be vaccinated against measles.
Due to generally high vaccination rates, measles in Florida is rare but occurs every year and is most often associated with international travel. So far in 2019, the one confirmed case had recent international travel to the Philippines.
National and International activity
Even though measles has been eliminated in the United States since 2000, cases occur every year, mostly among unvaccinated individuals. As of March 28, 387 confirmed cases of measles have been reported by 15 states and the District of Columbia in 2019. The 2-dose measles vaccination schedule has been successful at decreasing cases.
Recently, increased measles activity has been reported all over the world. The Centers for Disease Control and Prevention (CDC) issued a Level 1 Travel Alert for several countries with measles outbreaks, including the Philippines. Travelers to these countries should make sure they are vaccinated against measles with the MMR (measles, mumps, and rubella) vaccine. For more information, please visit CDC’s Travel Health
Florida Department of Health Officials Stress Importance of Awareness and Prevention of Hepatitis A
April 12, 2019
Communications Office
NewsMedia@flhealth.gov
(850) 245-4111Stuart, Fla. — Today, officials from the Florida Department of Health (DOH) in Tallahassee and Martin County (DOH–Martin) joined Lieutenant Governor Jeanette Nuñez, Florida Senator Gayle Harrell, Congressman Brian Mast, and local elected officials for a press conference to discuss the recent outbreak of hepatitis A in Martin County and across the state.
During the press conference, DOH officials announced that they have published a new webpage, www.floridahealth.gov/hepa, to educate Floridians on how you can protect yourself from hepatitis A and the steps you can take to prevent the spread of infection. They have also provided a dedicated phone line, 1-844-CALL-DOH (844) 225-5364), and a dedicated email inbox, hepa@flhealth.gov, for any concerns regarding hepatitis A.
“I want to assure Martin County residents that that we are diligently working to investigate the cause of these local hepatitis A infections and will leave no stone unturned,” said Lieutenant Governor Jeanette Nuñez. “The cases we are seeing in Florida are part of a national outbreak since 2017. As we investigate, we are working to educate the public about how they can best respond to this situation. Hepatitis A is rarely fatal and getting vaccinated is the single most important action people at risk can take to avoid getting hepatitis A.”
“With Florida being the third largest state in the country, it is unfortunate, but not surprising that our case numbers have also been rising,” said Dr. Carina Blackmore, the Florida State Epidemiologist. “As we continue with our investigation in Martin County, it is important to understand that hepatitis A is a vaccine-preventable liver disease. If you believe you may have hepatitis A, please consult with your doctor, especially if you have underlying health problems such as chronic liver or kidney disease or a weak immune system.”
About Hepatitis A
Hepatitis A is a vaccine-preventable liver disease. While normally not fatal, persons with chronic liver or kidney disease or compromised immune systems are more likely to experience a severe illness, leading to liver failure and possible death.
Since February, 2019, 19 persons with hepatitis A, a contagious liver disease, have been reported in Martin County. Fourteen persons have been hospitalized, and three have passed away due to complications related to hepatitis A infection. Infected persons range in age from 27 to 87 years. Eight persons are known to be linked to others that had hepatitis A and five people report additional risks for hepatitis A infection including drug use and homelessness.
Since January 2018, 1,293 cases of hepatitis A have been reported statewide. This increase in cases reflects national trends, as local and state health departments across the country have worked closely with the Centers for Disease Control and Prevention (CDC) to respond to similar outbreaks since March 2017.
During each investigation, DOH-Martin conducts interviews to identify close contacts of the ill person who should receive the hepatitis A vaccine to prevent disease. Additionally, DOH-Martin reviews if common activities have occurred among cases in the 50 days prior to persons becoming ill. No common shared activities, including restaurants, have been identified at this time but investigations are ongoing.
Hepatitis A is transmitted from person-to-person through contact with an infected person’s feces (poop). This can result from poor hand washing after going to the bathroom. Hepatitis A can also be spread through food or water contaminated with fecal matter or during close contact with others, such as sexual contact. While most patients with hepatitis A will fully recover, some may require hospitalization. Deaths rarely occur.
The symptoms of hepatitis A can include: fever, jaundice (yellow skin and eyes), tiredness, loss of appetite, vomiting, abdominal pain, dark urine, diarrhea, and gray clay-colored stool. If you have symptoms of hepatitis A, you should visit your health care provider for evaluation. People that are exposed to hepatitis A may be given vaccine or immune globulin within 14 days of exposure to prevent infection.
DOH recommends that health care providers offer hepatitis A vaccine to all persons at risk of hepatitis A infection who have not been vaccinated or do not know their vaccination status.
Health care providers are also asked to immediately report all cases of hepatitis A to their local county health department to ensure a prompt public health response to prevent disease among close contacts.
For more information on the Florida hepatitis A outbreak visit www.floridahealth.gov/hepa.
If you have any questions or concerns, you can email hepa@flhealth.gov or call 1-844-CALL-DOH (844) 225-5364) during normal operating hours.
About the Florida Department of Health
The department, nationally accredited by the Public Health Accreditation Board, works to protect, promote and improve the health of all people in Florida through integrated state, county and community efforts.
Follow us on Twitter at @HealthyFla and on Facebook. For more information about the Florida Department of Health please visit www.FloridaHealth.gov.
CDC-Cut Fruit SalmenallaNotices webpage.
CDC, public health and regulatory officials in several states, and the U.S. Food and Drug Administration are investigating a multistate outbreak of Salmonella Carrau infections linked to pre-cut melons supplied by Caito Foods LLC.

- Reported Cases: 93
- States: 9
- Hospitalizations: 23
- Deaths: 0
- Recall: Yes
Do not eat, serve, or sell recalled pre-cut melon and fruit medley products produced by Caito Foods, LLC and sold under several brands and labels.
- On April 12, 2019, Caito Foods LLC recalledExternal pre-cut watermelon, honeydew melon, cantaloupe, and pre-cut fruit medley products containing one of these melons supplied at the Caito Foods LLC facility in Indianapolis, Indiana.
- These products were distributed in Illinois, Indiana, Iowa, Kansas, Kentucky, Michigan, Minnesota, Missouri, Nebraska, New York, North Carolina, Ohio, Pennsylvania, Tennessee, West Virginia, and Wisconsin.
- Check FDA’s websiteExternal for a full list of where recalled products were sold.
- Recalled pre-cut melons were packaged in clear, plastic clamshell containers.
- Caito Foods LLC and SpartanNash Company (a Caito Foods LLC distributor) supply to independent retailers, so it is important to look at the label description and brand information to identify the product.
- If you cannot determine if pre-cut melon you purchased was produced by Caito Foods LLC, don’t eat it and throw it away.
- Check your fridge and freezer for recalled products and throw them away or return them to the place of purchase for a refund. Follow these steps to clean your fridge if you had any recalled product.
- CDC will update the advice to consumers and retailers when more information is available.
Contact a healthcare provider if you think you got sick from consuming pre-cut melon.
- Most people infected with Salmonella develop the following signs and symptoms 12 to 72 hours after eating a contaminated product:
- Diarrhea
- Fever
- Abdominal cramps
- A total of 93 people infected with the outbreak strain of Salmonella Carrau have been reported from 9 states.
- Illnesses started on dates ranging from March, 4, 2019, to March, 31, 2019.
- 23 people have been hospitalized. No deaths have been reported.
- Most of the ill people are adults over the age of 50.
- Epidemiologic and traceback evidence indicates that pre-cut melons supplied by Caito Foods LLC are the likely source of this outbreak.
- On April 12, 2019, Caito Foods LLC recalledExternal pre-cut watermelon, honeydew melon, cantaloupe, and pre-cut fruit medley products containing one of these melons produced at the Caito Foods LLC facility in Indianapolis, Indiana.
- This investigation is ongoing, and CDC will provide updates when more information is available.

- Most people infected with Salmonella develop diarrhea, fever, and stomach cramps 12 to 72 hours after being exposed to the bacteria.
- The illness usually lasts 4 to 7 days, and most people recover without treatment.
- In some people, the illness may be so severe that the patient needs to be hospitalized. Salmonellainfection may spread from the intestines to the bloodstream and then to other places in the body.
- Children younger than 5 years, adults older than 65 years, and people with weakened immune systems are more likely to have a severe illness.
April 12, 2019
CDC, public health and regulatory officials in several states, and the U.S. Food and Drug Administration are investigating a multistate outbreak of Salmonella Carrau infections.
Public health investigators are using the PulseNet system to identify illnesses that may be part of this outbreak. PulseNet is the national subtyping network of public health and food regulatory agency laboratories coordinated by CDC. DNA fingerprinting is performed on Salmonella bacteria isolated from ill people by using techniques called pulsed-field gel electrophoresis (PFGE) and whole genome sequencing (WGS). CDC PulseNet manages a national database of these DNA fingerprints to identify possible outbreaks. WGS gives a more detailed DNA fingerprint than PFGE. WGS showed that isolates from ill people were closely relatedly genetically. This means that people in this outbreak were more likely to share a common source of infection.
The multistate investigation began on April 2, 2019, when PulseNet identified the outbreak. As of April 12, 2019, 93 people infected with the outbreak strain of Salmonella Carrau have been reported from nine states. A list of the states and the number of cases in each can be found on the Map of Reported Cases page.
Illnesses started on dates ranging from March 4, 2019, to March 31, 2019. Ill people range in age from less than one to 98 years, with a median age of 53. Fifty-seven percent are female. Of 53 people with information available, 23 (43%) have been hospitalized. No deaths have been reported.
Illnesses might not yet be reported due to the time it takes between when a person becomes ill and when the illness is reported. This takes an average of 4 weeks. Please see the Timeline for Reporting Cases of Salmonella Infection for more details.
Investigation of the Outbreak
Epidemiologic and traceback evidence indicate that pre-cut melon supplied by Caito Foods LLC of Indianapolis, Indiana is the likely source of this multistate outbreak.
In interviews, ill people answered questions about the foods they ate and other exposures in the week before they became ill. Thirty (77%) of 39 people interviewed reported eating pre-cut melons purchased from grocery stores, including pre-cut cantaloupe, watermelon, honeydew, or a fruit salad mix or fruit tray with melon. Four additional people reported eating pre-cut melon outside the home.
Information collected from stores where ill people shopped indicates that Caito Foods LLC supplied pre-cut melon to these stores. On April 12, 2019, Caito Foods, Inc. recalledExternal pre-cut watermelon, honeydew melon, cantaloupe, and pre-cut fruit medley products containing one of these melons produced at the Caito Foods LLC facility in Indianapolis, Indiana.
This investigation is ongoing, and CDC will provide updates when more information is available.
E-COLI-Timeline of Reported Cases
Posted April 12, 2019 at 3:15 PM ET
People infected with the outbreak strain of E. coli O103, by date of illness onset*
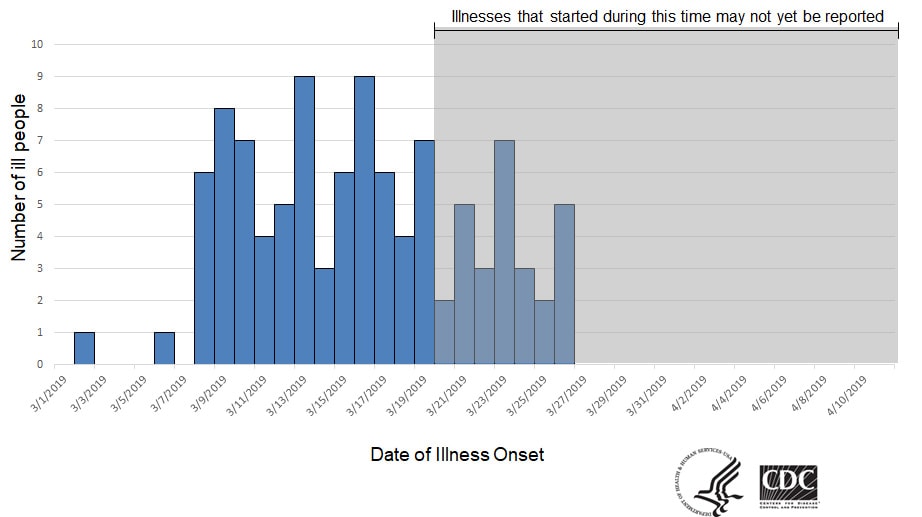
*n=103 for whom information was reported as of April 12, 2019. Some illness onset dates have been estimated from other reported information.